Survey Of Pediatric Gastrointestinal Endoscopy Practice Patterns In Children – 2018.
https://goo.gl/forms/d5suYmxiCwiOQDXS2
Results Of The Worldwide Survey Of Current Digestive Endoscopy Practice in Children in 2018
Authors: Prévost Jantchou, Kiana Tchan, Noémie Laverdure, Lara Hart, Jennifer Ao, Mallory Chavannes
Institutions: CHU Sainte Justine / Université de Montréal, Paediatrics, Montreal, Canada, 2 Research center of CHU Sainte-Justine, Epidemiology, Montreal, Canada, 3 Montreal Children’s Hospital, Paediatrics, Montreal, Canada, 4 University of Southern California; Children’s Hospital of Los Angeles, Paediatrics, Los Angeles, United States
Background: Pediatric digestive endoscopies are invasive procedures that must be done by experienced physicians within an environment that ensures the safety of the patients. In recent years there have been an increase in the number of endoscopies performed on children due to the rising incidence of various intestinal diseases such as inflammatory bowel disease, coeliac disease or eosinophilic esophagitis.
Aim: to describe the current pattern of pediatric digestive endoscopy practice worldwide
Methods: An online questionnaire (43 questions) was developed on google form ™ and sent to pediatric gastroenterologists around the globe using the following steps: 1) the link was sent to all the subscribers of the PEDGI forum (Pediatric GI Bulletin Board); 2) targeted emails were sent using the directory of the French Speaking Group of Pediatric Hepatology and Gastroenterology and the ESPGHAN Africa mailing list; and 3) individual emails were sent by collecting email addresses of pediatric gastroenterologists through manual Pubmed search.
Results:
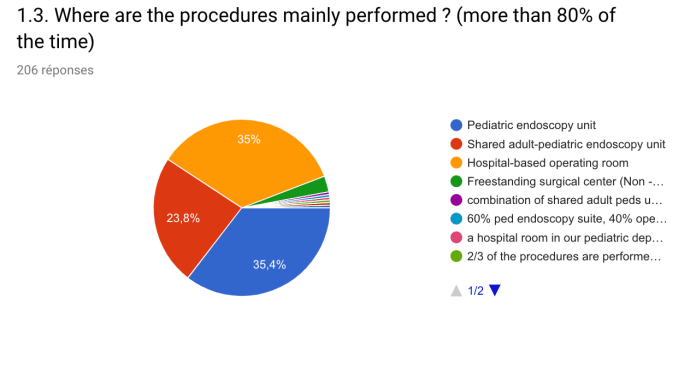
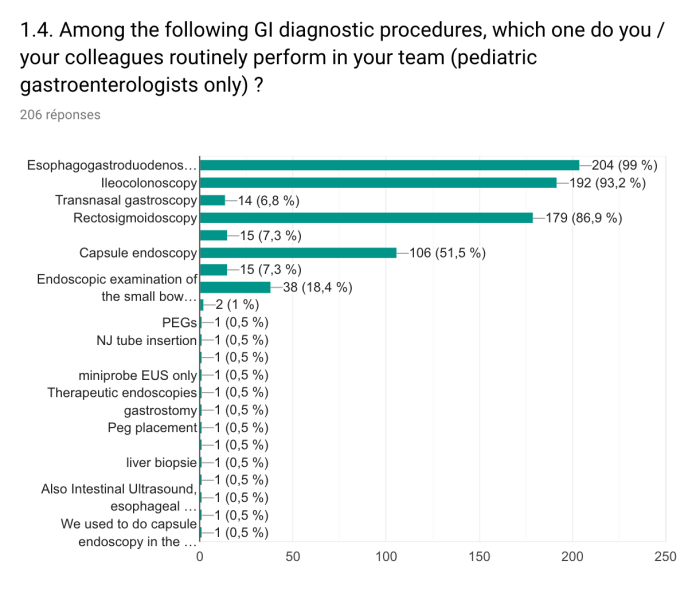
A total of 201 responses were received from 5 continents; 54 countries; 158 cities. Nearly all the centers (99%) performed diagnostic oesogastroduodenoscopies (OGD) and 192 (93.2%) performed ileocolonoscopy (COLO). The annual volume of procedures (OGD and COLO combined) varied highly between centers, with only 26% performing more than 1000 procedures annually.
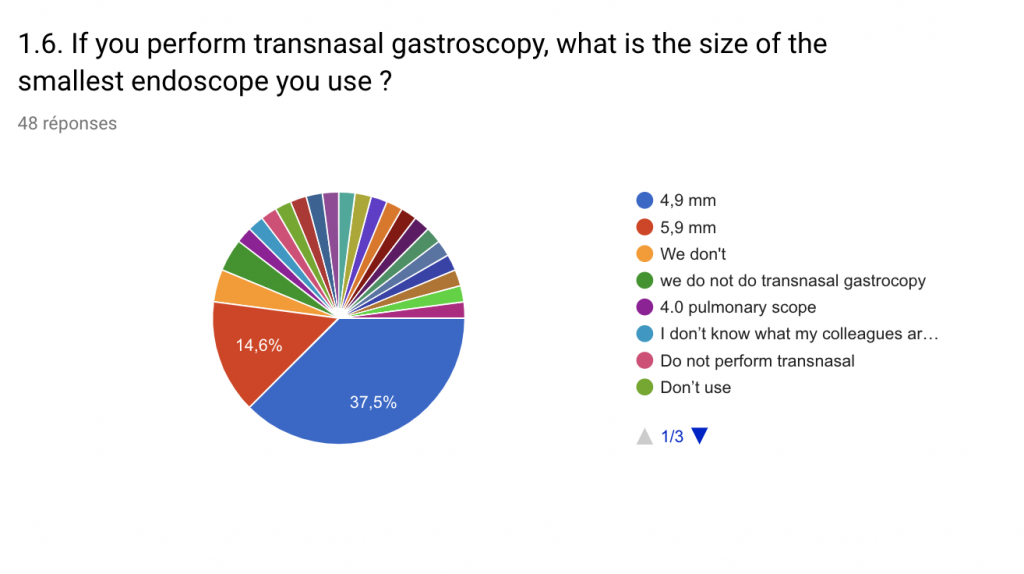
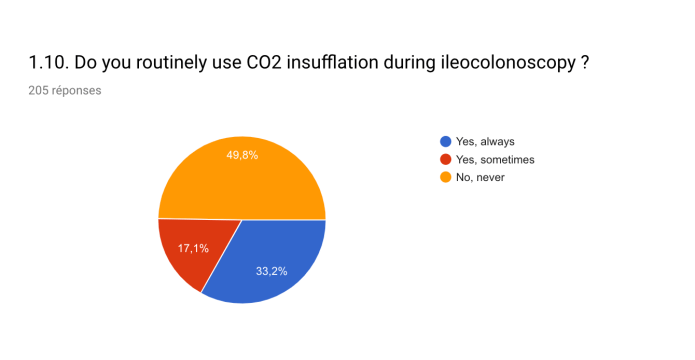
Ninety three percent of centers performed therapeutic procedures. The most common were polypectomies (93%), variceal ligation (77%) and oesophageal balloon dilatation (52.5%). Only 6.8% of respondents routinely performed transnasal gastroscopy. A scope guide was used in 13.0% of centers and CO2 insufflation for COLO was used by 50.2% of respondents.
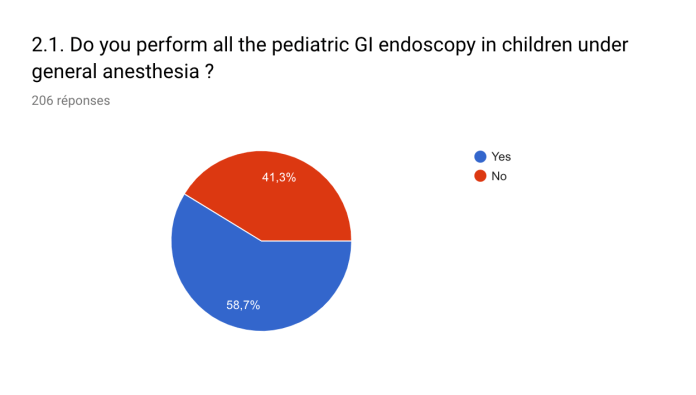
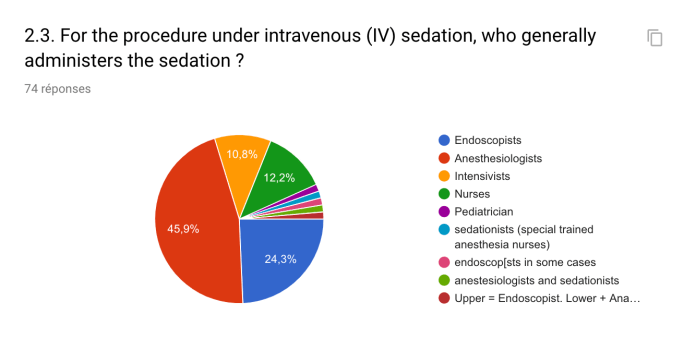
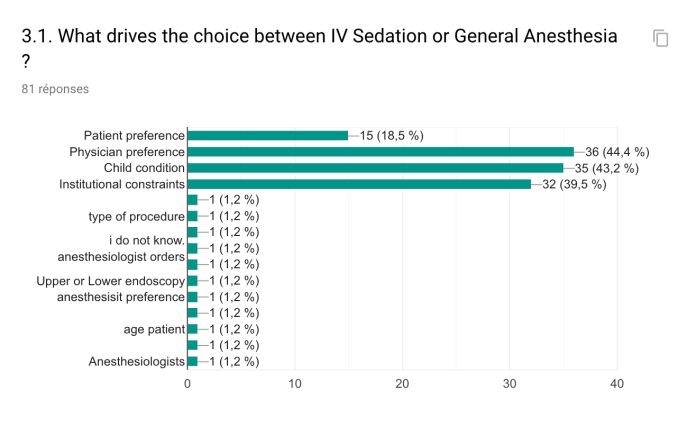
The methods of sedation for endoscopy varied between centers. Indeed, 58.7% of centers performed all procedures in children under general anesthesia (GA), 20.3% performed procedures under deep intravenous sedation (IVS) led by anesthesiologists and 20.0% performed procedures under sedation led by endoscopists. The choice between GA and IVS was driven by institutional constraints, patient preference, physician preference or child condition.
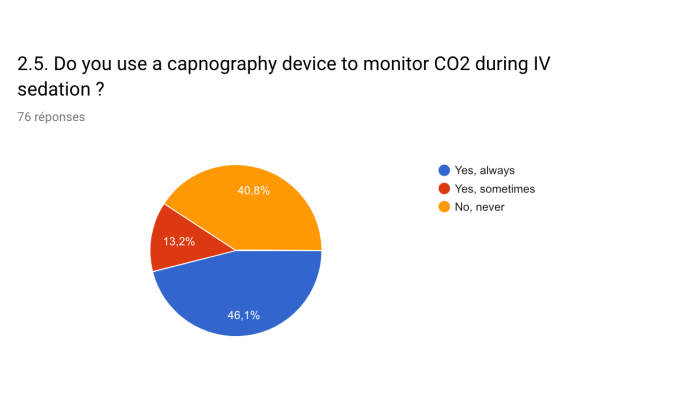
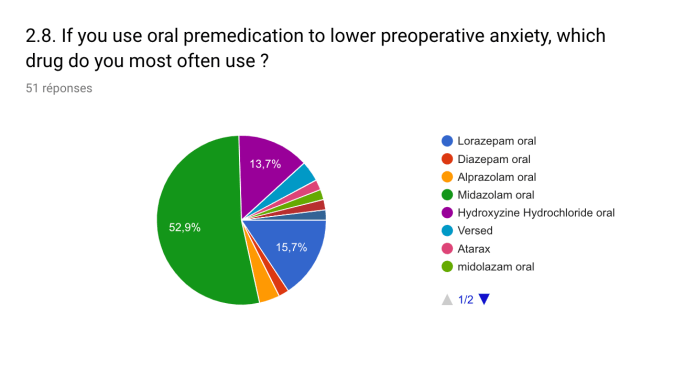
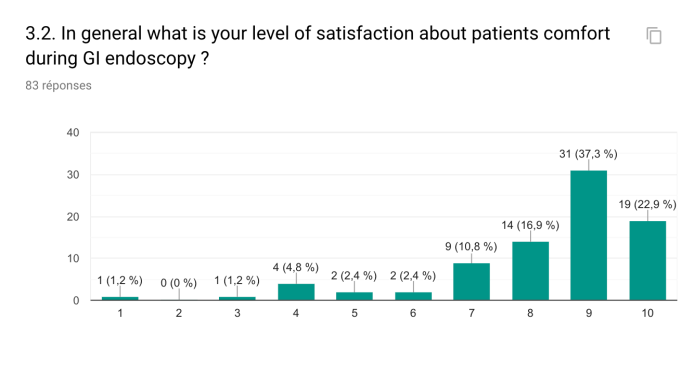
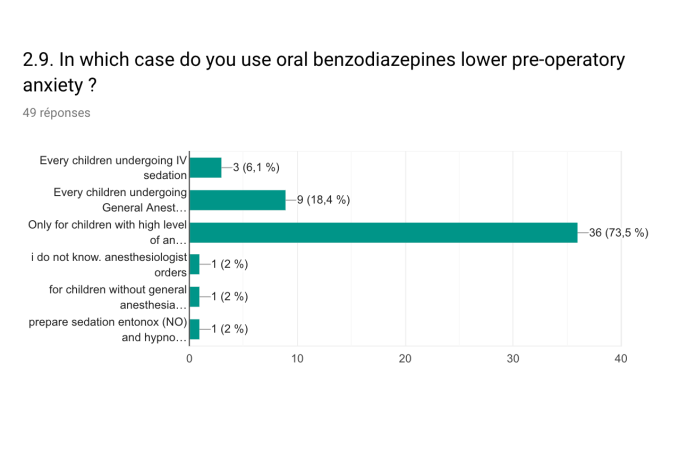
Midazolam and fentanyl were the two most common medications used by endoscopists for IVS. Propofol was routinely used by 57.5% of centers for anesthesiology-induced IVS. Oral benzodiazepine was administered to lower preprocedural anxiety in 26.8% of the centers. Only 56.1% of the respondents used a validated tool to evaluate the level of procedural pain or discomfort during IVS.
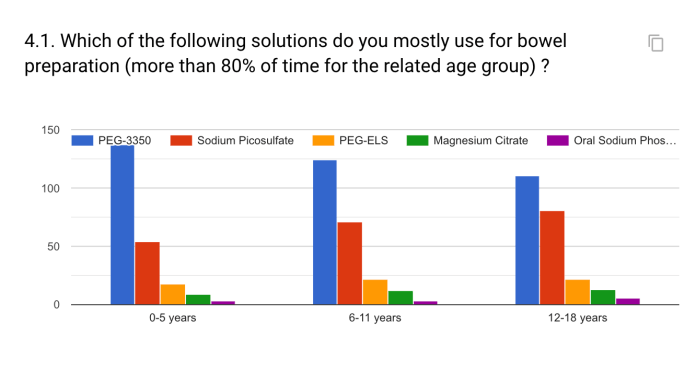
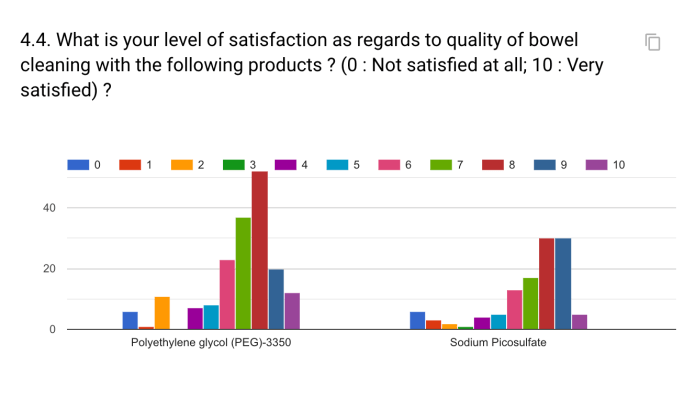
In order to assess the quality of bowel cleaning, validated scores such as Boston Bowel preparation Scale, Aronchick Bowel Preparation Scale or the Ottawa Bowel Preparation Scale were used in less than 40% of patients. A dedicated electronic reporting system was available in only 59.6% of centers.
Conclusion: The current survey is the first attempt to report a global mapping of pediatric endoscopy practices. There are some significant differences across centers and continents for the different measures. The evaluation of procedural pain/discomfort and the evaluation of bowel cleaning quality by validated scores are not routinely implemented in the majority of pediatric endoscopic rooms.
View MAPENDOWORLD in a full screen map